Overview
Did you know there are 12 cranial nerves in your body?
They work in pairs to establish connections between your brain and different parts of your body, like your head, neck, and torso.
Some of these nerves carry sensory information, relaying details about smells, sights, tastes, and sounds to your brain. These nerves are responsible for your senses.
On the other hand, certain cranial nerves control the movement of muscles and the function of glands. These nerves are in charge of motor functions.
The vagus nerve is responsible for carrying sensory and motor signals between the brain and the body, playing a crucial role in regulating many bodily functions.
Let’s explore more about it:
What is Vagus Nerve?
The vagus nerve, also known as the tenth cranial nerve or CN X, is one of the major nerves in the human body. It is a long and complex nerve that extends from the brainstem to various organs in the body, including the heart, lungs, stomach, and intestines.
The sensory nerve plays a big role in keeping our gut healthy. It controls the contraction of muscles in our intestines and sends messages to our brain and other important organs about what’s happening in our gut. This is known as the Brain-Gut Axis, and it helps to manage inflammation.
The vagus nerve, by regulating our breathing and heart rate, has a direct effect on how we respond to stress and how well we can relax.
The classification of cranial nerves uses Roman numerals to indicate their location.
Take a look at the diagram below to visualize the position of the vagus nerve.

When does the Vagus Nerve Develop?
The development of the vagus nerve occurs after birth. During the first year of life, an infant’s nervous system undergoes significant changes.
Initially, in the third trimester of pregnancy, the vagus nerve focuses on crucial functions like breathing, feeding, and regulating body temperature to adapt to life outside the womb.
As the infant grows, the vagus nerve continues to develop, allowing them to interact with their surroundings.
It enables physiological regulation of essential life functions, including breathing, eating, and heart rate.
This development throughout the first year enables infants to engage with objects, people, and their environment more actively.
What does the Vagus Nerve Control?

The vagus nerve, also known as the pneumogastric nerve, affects several important functions in the body, including:
Digestion: It plays a role in regulating digestive processes, such as the release of enzymes and the movement of food through the digestive system.
Heart rate: It helps regulate heart rate, promoting a balanced and healthy rhythm.
Breathing: It influences breathing patterns and helps control the rate and depth of respiration.
Cardiovascular activity: The vagus nerve contributes to the regulation of blood pressure and cardiovascular functions.
Reflex actions: It is involved in reflex actions like coughing, sneezing, swallowing, and vomiting.
The vagus nerve is part of the autonomic nervous system, which manages involuntary actions in the body, including breathing and digestion.
How the Vagus Nerve Is Central to Infant Emotional Development

The vagus nerve is vital for infant emotional development. It regulates the autonomic nervous system, shaping emotional responses.
It helps establish bonding, promotes self-regulation, and influences long-term emotional well-being.
Higher vagal tone is linked to better emotional regulation and secure attachment, while lower tone may lead to difficulties.
Nurturing positive experiences and supportive caregiving are crucial for healthy vagal functioning and emotional resilience in infants.
Effects on Emotional Development
As mammals, we are unable to take care of ourselves independently, relying on others for a safe environment.
Our emotional development and the strength of our vagus nerve are greatly influenced by the care we receive from others.
When our basic needs, as well as our social and emotional needs, are met in a loving environment, it contributes to the development of a strong or high vagal tone.
This positive foundation facilitates a smooth transition from dependency on caregivers to becoming well-adjusted, independent individuals in adolescence and adulthood.
Problems with the Vagus Nerve

When the vagus nerve is damaged, it can lead to various symptoms due to its extensive reach and impact on multiple areas of the body.
Some potential symptoms of vagus nerve damage include:
- Difficulty speaking or changes in voice.
- Difficulty swallowing or loss of the gag reflex.
- Low blood pressure or fluctuations in heart rate (either slow or fast).
- Digestive issues, such as changes in the digestive process, nausea, vomiting, abdominal bloating, or pain.
- Depression and anxiety in individuals with breathing problems or heart disease.
The specific symptoms experienced depend on the location of the nerve damage.
Heart Rate Issues
Vagal nerve dysfunction can result in both slow (bradycardia) and fast (tachycardia) heart rates, depending on the type of dysfunction.
Overactivity of the vagus nerve can lead to a slow heart rate, while inadequate activity can cause a fast heart rate.
In some cases, vagal nerve maneuvers may be used to stimulate more vagal nerve activity and slow down the heart rate.
Gastroparesis
Damage to the vagus nerve can contribute to a condition called gastroparesis, which affects the involuntary contractions of the digestive system and impairs stomach emptying.
Gastroparesis can sometimes occur after a vagotomy procedure, which involves the removal of all or part of the vagus nerve.
Vasovagal Syncope
The vagus nerve stimulates certain heart muscles involved in slowing down the heart rate. If the vagus nerve overreacts, it can cause a sudden drop in heart rate and blood pressure, resulting in fainting episodes known as vasovagal syncope.
Triggers for this condition can include pregnancy, emotional stress, pain, or may occur without a clear cause. Alongside fainting, symptoms may include
- warmth
- nausea
- tunnel vision
- ringing in the ears
- excessive sweating
- low blood pressure
- slow or irregular heartbeat.
If experiencing fainting, it’s advisable to consult a doctor to rule out serious underlying causes.
Preventive measures may include staying well-hydrated or avoiding rapid changes in posture.
Vagus Nerve Stimulation (VNS)
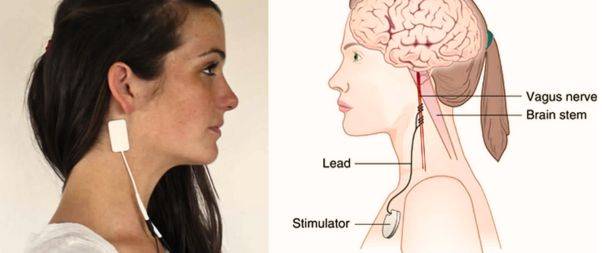
VNS is a treatment method that involves using electrical impulses to stimulate the vagus nerve. It is primarily used for cases of epilepsy and depression that do not respond to other treatments.
Researchers believe that the vagus nerve may play a role in linking depression, metabolic diseases, and heart disease. If ongoing research confirms this connection, VNS could potentially offer benefits for a variety of health issues.
During the VNS procedure, a device is typically implanted beneath the skin of the chest, and a wire connects it to the left vagus nerve. Once activated, the device sends signals through the vagus nerve to the brainstem, relaying information to the brain.
A neurologist usually programs the device, but individuals often receive a handheld magnet that allows them to control the device themselves.
It is believed that VNS holds potential for treating other conditions in the future, such as
- Multiple sclerosis
- Posterior autoimmune uveitis
- Alzheimer’s disease
- cluster headaches
However, further research is required to explore the effectiveness of VNS for these conditions.
Ongoing Research and Considerations
Researchers are actively investigating the vagus nerve as it holds potential clues to various health issues.
Here are some areas of interest:
Mental health and well-being: There is interest in exploring different methods of stimulating the vagus nerve to improve mental well-being and manage depression. Techniques such as diaphragmatic breathing, cold water immersion, transcutaneous VNS devices, biofeedback, and yoga have been explored. However, the safety and effectiveness of these methods for everyone are not yet fully established, and it is important to consult a doctor before trying new treatments.
Aging and vagal response: Research suggests that vagal response decreases with age. Individuals with a strong vagal tone may find it easier to relax after stressful events, exhibit better management of inflammation and gut issues, and potentially have improved blood sugar regulation. However, further research is needed to validate these findings.
Rheumatoid arthritis (RA): There is some evidence that VNS may help reduce the severity of RA, an inflammatory condition affecting the joints. A study in 2021 found that individuals using a VNS device for 12 weeks experienced meaningful reductions in inflammation markers. However, more research is required to determine the safety and efficacy of VNS in managing Rheumatoid arthritis across a broader population.
It is essential to keep in mind that while these areas show promise, further research is necessary to establish the effectiveness, safety, and applicability of VNS and related techniques for specific conditions and individuals.
Consulting with a healthcare professional is crucial before attempting any new treatment strategy.
5 Ways to Activate The Vagus Nerve
Here are five effective ways to activate the vagus nerve:
Deep Breathing: Engage in slow, deep breaths by inhaling deeply through your nose and exhaling slowly through your mouth. This type of diaphragmatic breathing stimulates the vagus nerve and promotes relaxation and stress reduction.
Cold Exposure: Brief exposure to cold temperatures, such as taking cold showers or splashing cold water on your face, can activate the vagus nerve. The shock of cold triggers a natural physiological response that stimulates the nerve and enhances its function.
Singing or Chanting: Vocal exercises like singing or chanting involve controlled breath and vibration, which stimulate the vagus nerve. This practice can help regulate your heart rate and promote a sense of calm and well-being.
Meditation or Mindfulness: Engaging in meditation or mindfulness practices has been shown to activate the vagus nerve. Focusing on the present moment, deep breathing, and cultivating a state of relaxation can enhance vagal tone and overall well-being.
Yoga or Tai Chi: These mind-body practices combine deep breathing, gentle movements, and relaxation techniques, all of which can activate the vagus nerve. Yoga poses, such as backbends or inversions, are particularly effective in stimulating the nerve.
It’s important to note that the effectiveness of these methods may vary from person to person, and it’s always a good idea to consult with a healthcare professional before trying new techniques, especially if you have any underlying health conditions.
Take Care of Yourself!
Also Read