Cervical cancer is a significant health concern affecting women worldwide. Detecting and diagnosing cervical cancer at an early stage is crucial for successful treatment and improved outcomes.
One powerful diagnostic tool used in the evaluation of cervical cancer is ultrasound imaging.
In this article, we will explore what cervical cancer looks like on an ultrasound and understand its role in diagnosis and monitoring.
Understanding Ultrasound Imaging
Ultrasound imaging, also known as sonography, is a non-invasive imaging technique that uses high-frequency sound waves to create real-time images of the body’s internal structures.
It is a safe and widely used diagnostic tool for assessing various medical conditions, including cervical cancer.
Ultrasound and Cervical Cancer
When it comes to cervical cancer, ultrasound can provide valuable information about the size, shape, and characteristics of the tumor. Although ultrasound is not typically the primary screening tool for cervical cancer, it is often used in conjunction with other diagnostic tests like Pap smears and colposcopy.
Transvaginal Ultrasound

For evaluating cervical cancer, transvaginal ultrasound is the preferred approach.
In this procedure, a small probe called a transducer is inserted into the vagina, allowing for a closer examination of the cervix and surrounding structures.
The transducer emits sound waves that bounce back from the tissues, creating a detailed image on the ultrasound monitor.
What Does Cervical Cancer Look Like on an Ultrasound?

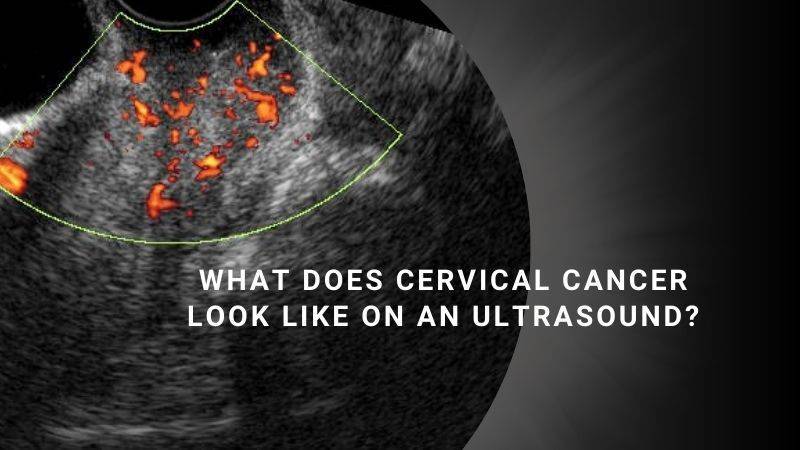
On an ultrasound image, cervical cancer may appear as a mass or a growth in or around the cervix. The tumor can vary in size, shape, and texture.
The ultrasound can help determine if the mass is localized or has spread to nearby structures, such as the uterus or lymph nodes.
Characteristics of Cervical Cancer on Ultrasound
- Irregular Borders: Cervical cancer often exhibits irregular, poorly defined borders on ultrasound. This can indicate invasive growth into surrounding tissues.
- Increased Vascularity: Cancerous tumors require a rich blood supply to sustain their growth. On ultrasound, cervical cancer may show increased blood flow, indicated by areas of increased vascularity or Doppler signals.
- Distortion of Cervical Anatomy: Cervical cancer can cause structural changes in the cervix. Ultrasound can help identify these distortions, such as irregularities in the shape or size of the cervix.
- Presence of Lymph Nodes: Ultrasound can also detect enlarged lymph nodes in the pelvis, which may indicate the spread of cervical cancer to these regions.
Limitations of Ultrasound in Cervical Cancer Diagnosis
While ultrasound is a valuable imaging tool, it does have certain limitations in diagnosing cervical cancer.
It cannot definitively confirm or rule out the presence of cancer. In cases where abnormalities are detected, further diagnostic tests such as biopsies may be necessary to obtain a conclusive diagnosis.
Is Ultrasound Effective for Detecting Cervical Cancer?
When it comes to the detection and diagnosis of cervical cancer, ultrasound is not the primary screening tool.
While ultrasound is commonly used in obstetrics and gynecology to monitor fetal development during pregnancy and identify various growths like fibroids and cysts, it is not the most reliable method for detecting cervical cancer.
Ultrasound imaging uses sound waves to create images of the internal structures of the body. While certain types of ultrasound tests may show signs of specific types of cervical cancer, it is unlikely for healthcare professionals to identify cervical cancer during an unrelated ultrasound exam.
The primary purpose of an ultrasound may not involve the identification of cervical cancer, and ultrasound technicians may not be specifically trained to recognize this particular type of cancer.
More Reliable Methods for Screening and Diagnosing Cervical Cancer

Pap Smear Test: A Pap smear, also known as a Pap test, is a routine screening procedure used to detect abnormal cervical cells that may indicate the presence of cervical cancer or precancerous changes.
HPV Test: The human papillomavirus (HPV) test detects the presence of high-risk strains of HPV, which can lead to cervical cancer. This test is often performed in conjunction with a Pap smear.
Colposcopy: If abnormalities are found during a Pap smear or HPV test, a colposcopy may be performed. This procedure involves examining the cervix and the surrounding tissues using a special magnifying instrument called a colposcope.
Biopsy: If suspicious areas are identified during a colposcopy, a biopsy may be recommended. This involves taking a small tissue sample from the cervix for further examination under a microscope to confirm the presence of cervical cancer.
Use of Ultrasound in Later Stages of Cervical Cancer Diagnosis
While ultrasound is not typically used for initial detection, it may be employed in the later stages of the cervical cancer diagnosis process.
After a cervical cancer diagnosis is confirmed through a biopsy, healthcare providers may recommend additional imaging tests, including ultrasound, to determine if the cancer has spread to nearby tissues or other parts of the body.
These tests help in staging the cancer and developing an appropriate treatment plan.
How Often Should You Get Screened for Cervical Cancer?

The recommended screening guidelines may vary depending on your age and previous screening results.
Here are the general guidelines provided by reputable sources like the American Cancer Society and the Centers for Disease Control and Prevention (CDC):
Age 21: It is recommended to start cervical cancer screening with Pap tests from the age of 21, regardless of sexual activity or HPV vaccination history.
Ages 21 to 29: If Pap test results are normal, it is generally recommended to have a Pap test every three years during this age range.
Ages 30 to 65: There are a few options available for screening during this period:
a. Pap test only: If results are normal, it is typically advised to have a Pap test every three years.
b. HPV test only: Alternatively, an HPV test can be done alone, without a Pap test. If the HPV test results are negative, it is generally recommended to have an HPV test every five years.
c. Pap and HPV co-test: Another option is to have both a Pap test and an HPV test together. If both results are normal, it is typically advised to undergo testing every five years.
Age 65 and above: If you have had consistently normal screening results in recent years and are not at high risk, further testing may not be necessary. However, it is important to consult with your healthcare provider to determine the most appropriate course of action based on your individual circumstances.
Additionally, it is essential to be aware of any unusual changes or symptoms between screenings.
If you experience
- abnormal spotting or bleeding
- heavy menstrual periods
- unusual vaginal discharge
- pelvic pain, or bleeding or discomfort after sex
It is important to inform your doctor and seek medical attention promptly.
Remember, these are general guidelines, and individual situations may vary. It is crucial to have regular discussions with your healthcare provider to determine the most suitable screening schedule based on your age, medical history, and risk factors.
Conclusion
While ultrasound is a valuable imaging tool used for various medical purposes, it is not the most effective method for screening and diagnosing cervical cancer.
Reliable methods such as Pap smears, HPV tests, colposcopy, and biopsies are preferred for early detection and diagnosis.
If you have concerns about cervical health or need to be screened for cervical cancer, it is important to consult with your healthcare provider who can guide you through the appropriate screening and diagnostic procedures.
Also Read